Often referred to as “liquid gold,” breast milk plays a vital role in nourishing infants, providing them with unparalleled benefits.
As a parent, it is crucial to grasp the remarkable advantages of breastfeeding and the remarkable composition of breast milk.
In this all-inclusive guide, we will explore the multitude of benefits offered by breast milk, draw a comparison between breast milk and cow’s milk, and address prevalent concerns and misconceptions about human milk.
Ready to roll?
The Importance of Breast Milk

Breast milk has long been recognized as the optimal source of infant nutrition.
Its unique composition is tailored to meet the needs of growing babies, providing a wide range of essential nutrients, antibodies, and bioactive compounds.
Breast milk is easily digestible, promotes healthy development, and offers numerous long-term health benefits.
The Power of Breast Milk Antibodies
Breast milk possesses an exceptional attribute: the capacity to fortify infants with a resilient immune system.
Immunoglobulins, commonly referred to as antibodies, are abundantly present in breast milk and play a vital role in shielding babies against many infections and diseases.
By transferring these antibodies from mother to baby, breast milk bolsters their immune response and diminishes the likelihood of respiratory, gastrointestinal, and ear infections.
This extraordinary defense mechanism is a testament to the remarkable protective power of breast milk.
Enhanced Cognitive Development
Breast milk is nourishing and crucial in promoting optimal brain development. It contains essential fatty acids, such as docosahexaenoic acid (DHA), which are vital for the growth and function of the nervous system.
Studies have shown that breastfed infants may have improved cognitive abilities and a reduced risk of developmental delays compared to formula-fed babies.
Emotional Bonding and Maternal Health
Breastfeeding fosters a unique bond between mother and child, creating a deep emotional connection.
The act of nursing releases oxytocin, often referred to as the “love hormone,” which promotes feelings of relaxation, trust, and bonding.
Additionally, breastfeeding offers numerous health benefits for mothers, including a reduced risk of postpartum hemorrhage, faster postpartum recovery, and a lower likelihood of developing certain types of cancer.
Composition of Breast Milk
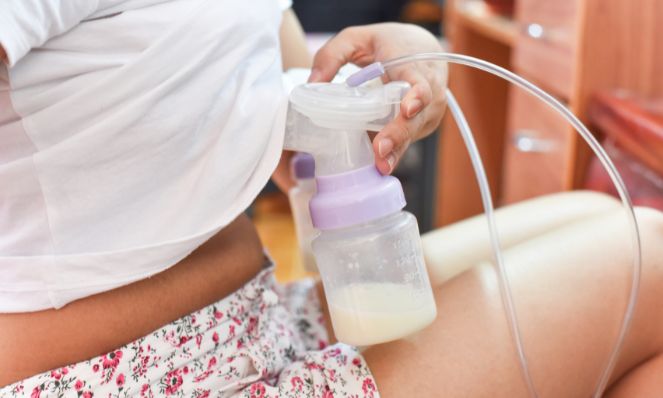
Breast milk is a complex, dynamic fluid that adapts to the changing needs of a growing baby.
Its composition varies throughout the day, between feedings, and even as the child ages.
Understanding the components of breast milk is key to appreciating its nutritional value.
Macronutrients (Protein, Fat, and Carbohydrates)
Breast milk offers a perfect blend of macronutrients crucial for the growth and development of infants.
The protein found in breast milk is easily digestible and supplies the essential building blocks for tissue growth.
Fat, serving as a vital energy source, plays a pivotal role in brain development and facilitates the absorption of fat-soluble vitamins.
Carbohydrates, predominantly lactose, provide energy and contribute to the healthy development of the central nervous system.
Micronutrients (Vitamins and Minerals)
Breast milk is rich in various vitamins and minerals essential for overall health and development.
Although breast milk usually provides adequate nutrition for infants, it is often advised to supplement with vitamin D.
While breast milk does contain vitamins and minerals like iron and calcium, additional dietary sources may be necessary as the child grows.
Bioactive Compounds and Hormones
Beyond its macronutrient and micronutrient content, breast milk is rich in bioactive compounds and hormones that support various aspects of infant health.
These include prebiotics that nourish beneficial gut bacteria, enzymes that aid in digestion, and growth factors that promote healthy tissue development.
Breast Milk vs. Cow’s Milk

Although breast milk is considered the ideal choice for infant nutrition, it’s natural for parents to question the suitability of cow’s milk as an alternative.
Now, let’s delve into the primary distinctions between these two milk options.
Protein Digestibility
Cow’s milk contains proteins, such as beta-lactoglobulin, that can be allergenic and more challenging for infants to digest.
In contrast, breast milk is easily digested and less likely to trigger allergic reactions.
This is especially advantageous for babies with a family history of allergies or those who are prone to gastrointestinal discomfort.
Carbohydrate Content and Digestion
The carbohydrate content in breast milk is naturally lower than that found in cow’s milk, largely due to the presence of lactose.
Lactose plays a crucial role in facilitating the absorption of vital minerals such as calcium and supports the growth of beneficial gut bacteria.
One remarkable aspect of breast milk is its consistent carbohydrate composition, which remains stable regardless of the mother’s diet.
This consistency ensures a reliable and steady energy source for the baby.
Fat Composition and Essential Fatty Acids
Breast milk boasts a higher fat content than cow’s milk, supplying the essential energy required for a growing infant.
It is abundant in unsaturated fatty acids, including DHA and arachidonic acid, which are critical for brain and vision development.
Furthermore, breast milk naturally contains cholesterol, a vital component for hormone synthesis and the maturation of the nervous system.
Vitamin and Mineral Profile
Breast milk provides infants an optimal balance of vitamins and minerals, except for vitamin D.
While breast milk contains some vitamin D, supplementation is typically recommended to meet the baby’s needs.
Cow milk, on the other hand, requires fortification to match the nutrient profile of breast milk.
Advantages of Breastfeeding

Breastfeeding provides a multitude of benefits for both infants and mothers.
Let’s take a closer look at the significant advantages that make breastfeeding the preferred option for infant nutrition!
Optimal Nutrition and Digestibility
Breast milk provides complete nutrition perfectly tailored to the needs of a growing baby.
Its composition evolves to meet the changing nutritional requirements of the child, ensuring optimal nutrient intake.
The easily digestible nature of breast milk minimizes the risk of gastrointestinal issues and promotes healthy weight gain.
Immune System Protection
Breast milk contains a myriad of immune-boosting properties that help protect infants from infections and diseases.
The antibodies present in breast milk provide passive immunity, safeguarding the baby’s health during the vulnerable early months.
Breastfed infants often experience fewer respiratory, gastrointestinal, and ear infections.
Long-Term Health Benefits
Breastfeeding has many long-term health benefits for both infants and mothers.
Breastfed babies have a reduced risk of developing conditions like asthma, allergies, obesity, and certain childhood cancers.
Mothers who breastfeed are less likely to develop ovarian or breast cancer and a decreased risk of type 2 diabetes and cardiovascular diseases.
Emotional Bonding and Maternal Health
Breastfeeding nurtures a unique emotional bond between mother and child.
Physical closeness and skin-to-skin contact during nursing promote feelings of security and attachment.
Additionally, breastfeeding stimulates the release of oxytocin, the hormone responsible for maternal bonding and reducing stress levels.
Environmental and Economic Benefits
Breastfeeding is not only beneficial for infants and mothers but also for the environment.
It is a sustainable practice that reduces the need for infant formula production, packaging, and transportation.
Breastfeeding also offers significant cost savings, eliminating the need to purchase expensive formula and feeding equipment.
Common Breastfeeding Concerns
Despite the numerous benefits of breastfeeding, many parents have concerns and face challenges along their breastfeeding journey.
Let’s address some common problems and provide guidance for overcoming them.
Milk Supply and Nursing Difficulties
One common concern is the adequacy of the milk supply.
While some mothers may experience challenges with breastfeeding and milk production, most women can produce enough milk to meet their baby’s needs with the right support and techniques.
Establishing a proper latch, practicing skin-to-skin contact, and seeking guidance from a lactation consultant can help address nursing difficulties and ensure a sufficient milk supply.
Returning to Work and Pumping
Balancing breastfeeding with work commitments can be challenging.
However, many mothers successfully continue breastfeeding after returning to work by planning, creating a pumping schedule, and utilizing supportive workplace policies.
Pumping breast milk allows mothers to provide their babies with the benefits of breast milk even when they are apart.
Breastfeeding and Medications
Another concern is the compatibility of breastfeeding with medications.
While some medicines may require caution or temporary interruption of breastfeeding, many drugs are safe to use while nursing.
Consulting healthcare professionals, such as lactation consultants or knowledgeable healthcare providers, can help determine the safety of specific medications during breastfeeding.
Related Post: Collagen and Breastfeeding: What You Need to Know
Breastfeeding and Special Circumstances
Breastfeeding is possible even in exceptional circumstances, such as premature birth, multiples, or medical conditions.
In these cases, seeking guidance from healthcare providers, lactation consultants, or support groups can provide valuable information and support tailored to individual circumstances.
Breast Milk Production and Supply

Understanding the factors influencing breast milk production and supply is vital for ensuring a successful breastfeeding journey.
Let’s explore the key aspects of milk production and strategies to maintain a healthy supply!
Supply and Demand: The Milk Production Feedback Loop
Breast milk production operates on a simple principle: supply and demand.
The more frequently and effectively the baby nurses, the more milk the mother’s body produces.
Establishing a consistent breastfeeding routine and ensuring the baby has unrestricted access to the breast helps maintain a healthy milk supply.
Increasing Milk Supply
If a mother experiences a low milk supply, there are various strategies to help increase production.
These include:
- Increasing the frequency of nursing or pumping sessions
- Practicing skin-to-skin contact
- Ensuring a proper latch and seeking support from lactation consultants or support groups.
Additionally, certain foods, such as oatmeal and fenugreek, are believed to have lactogenic properties and may help boost milk supply.
Managing Oversupply
While low milk supply can be a concern, some mothers may experience an oversupply of milk.
This can lead to engorgement, discomfort, and an overactive let-down reflex.
Strategies to manage oversupply include block feeding, using breast compression techniques, and seeking guidance from a lactation consultant.
Pumping and Storing Breast Milk
Pumping breast milk allows mothers to provide their babies with breast milk even when they are not physically present.
Proper pumping techniques, adequate storage, and safe handling of breast milk are essential to maintain its quality and ensure its safety for later use.
Breast Milk vs. Formula Feeding

While breastfeeding is widely recommended, formula feeding can be a viable option for some families.
Let’s explore the differences between breast milk and formula and considerations for choosing the most suitable feeding method!
Formula Feeding as an Alternative to Breast Milk
Formula milk is designed to mimic the nutritional composition of breast milk and provide essential nutrients required for infant growth.
It is made from cow’s milk, processed ingredients, and added supplements.
Formula feeding can be suitable for families who cannot breastfeed or choose not to.
Advantages of Formula Feeding
Formula feeding offers certain advantages, such as flexibility, allowing multiple caregivers to feed the baby.
It also provides a clear understanding of how much the baby consumes, making monitoring intake easier.
Additionally, formula feeding can be a practical solution for mothers with low milk supply or medical conditions that make breastfeeding painful.
Considerations for Choosing a Feeding Method
When deciding between breast milk and formula feeding, it is essential to consider individual circumstances, preferences, and the baby’s unique needs.
Breast milk provides unparalleled benefits and is the recommended choice whenever possible.
However, if formula feeding is chosen, selecting a suitable formula, consulting healthcare professionals, and practicing responsive feeding can help ensure the baby’s optimal nutrition and growth.
Introducing Cow’s Milk to Toddlers

Parents often wonder when and how to introduce cow’s milk as infants transition from breastfeeding or formula feeding to solid foods.
This section will explore the guidelines and considerations for introducing cow’s milk to toddlers.
Recommended Age for Introducing Cow’s Milk
The American Academy of Family Physicians (AAFP) recommends introducing cow’s milk as a primary beverage at around one year of age.
Before this age, breast milk or formula should remain the infants’ primary source of nutrition.
Introducing cow’s milk too early can increase the risk of allergies, gastrointestinal issues, and nutrient imbalances.
Nutritional Requirements for Toddlers
As infants transition to toddlerhood, their nutritional needs change.
Cow’s milk can be a valuable source of essential nutrients, such as calcium, protein, and vitamin D.
However, it is vital to ensure a balanced diet that includes a variety of foods rich in these nutrients, as well as fruits, vegetables, grains, and lean proteins.
Choosing the Right Type of Milk
When introducing cow’s milk, it is crucial to choose whole milk as a primary beverage for toddlers between the ages of one and two.
Whole milk provides the necessary fats for brain development and overall growth.
After age two, with guidance from healthcare professionals, low-fat or skim milk can be considered.
Alternatives for Children with Cow’s Milk Allergies or Dietary Restrictions
Some children may have allergies or intolerances to cow’s milk protein, or their families may follow a vegan lifestyle.
In such cases, healthcare professionals can suggest suitable milk alternatives, such as soy, almond, or oat.
It is important to ensure that these alternatives are fortified with calcium and vitamin D, as they may naturally contain lower levels of these nutrients.
Breast Milk Donation and Alternatives

Breast milk donation is an option for mothers unable to breastfeed or produce a sufficient milk supply.
Additionally, alternative feeding options are available for infants who cannot consume breast milk or formula.
Breast Milk Donation and Milk Banks
Breast milk donation involves providing excess breast milk to milk banks, which screen, pasteurize, and distribute the donated milk to infants in need.
This option allows babies to receive the benefits of breast milk even if their mothers cannot produce enough milk.
Donated breast milk is particularly valuable for premature babies or those with specific medical conditions.
Donor Milk and Informal Sharing
In addition to milk banks, some parents may explore informal milk-sharing arrangements, where breast milk is shared directly between individuals.
It is essential to exercise caution and ensure proper screening and testing to minimize potential risks associated with informal milk sharing.
Formula Feeding Alternatives
For infants who cannot consume breast milk or formula due to medical conditions or intolerances, specialized formulas are available.
These formulas are carefully formulated to provide the necessary nutrients and cater to specific dietary needs.
Consulting with healthcare professionals is crucial for determining the most suitable formula for such infants.
Frequently Asked Questions (FAQs)
How long does a woman have breast milk?
Breast milk production is a supply-and-demand process, meaning that the more the baby feeds or milk is removed, the more milk the body will produce. Most women are capable of producing milk as long as they continue this regular stimulation.
How long does it take for milk to replenish after pumping?
The time it takes for milk to replenish after pumping can vary from person to person. Generally, it can take about 20-30 minutes for the body to produce a significant amount of milk after a pumping session. However, milk production is continuous, and the supply gradually replenishes throughout the day. Consistently pumping on a regular schedule can help stimulate and maintain milk production.
Should I keep pumping if no milk is coming out?
If no milk is coming out while pumping, trying a few techniques to stimulate milk flow may be helpful, such as adjusting the pump settings or trying different pumping positions. However, if you consistently have difficulty expressing milk despite these efforts, seeking guidance from a lactation specialist or healthcare provider may be beneficial.
What foods help produce breast milk?
Certain foods can help increase breast milk production. These include oats, leafy greens, fenugreek, fennel, and whole grains. Maintaining a balanced diet, staying hydrated, and breastfeeding regularly for optimal milk supply is important.
Can I pump before the baby is born?
Yes, it is possible to pump before your baby is born. This process is known as antenatal or prenatal pumping. Some women choose to do this to establish a milk supply, particularly if they anticipate breastfeeding challenges or are planning to return to work shortly after giving birth.
Do leaking breasts mean they are full?
Leaking breasts do not necessarily indicate that they are full. Breast milk leakage can occur for various reasons, such as hormonal changes, let-down reflexes, or even pressure on the breasts. Some women may experience leakage even when their breasts are not overly full. On the other hand, some women may have full breasts without experiencing any leakage. It’s important to note that the feeling of fullness or engorgement, rather than leakage, is a more reliable sign of breast fullness.
What if my baby wants to nurse right after I pump?
If your baby wants to nurse right after you pump, it is perfectly fine to offer breastfeeding. Nursing provides more than just milk; it offers comfort, bonding, and important skin-to-skin contact. Your baby can still benefit from the breastfeeding session even if you have recently pumped.
Wrapping it Up
Breast milk is an excellent source of nutrition with numerous benefits for infants and mothers alike.
Its unique composition, tailored to meet the specific needs of a growing baby, provides optimal nutrition, immune protection, and long-term health advantages.
While breastfeeding is the recommended choice, formula feeding, and alternative feeding methods can be suitable options in specific circumstances.
By understanding the benefits of breast milk, addressing common concerns, and seeking support when needed, parents can make informed decisions about their child’s nutrition and provide the best start in life.
Remember, every parent’s journey is unique, and choosing what works best for you and your baby is the most important consideration.
Sources
- Liu, Z., Neuringer, M., Erdman, J. W., Jr, Kuchan, M. J., Renner, L., Johnson, E. E., Wang, X., & Kroenke, C. D. (2019). The effects of breastfeeding versus formula-feeding on cerebral cortex maturation in infant rhesus macaques. NeuroImage, 184, 372–385. https://doi.org/10.1016/j.neuroimage.2018.09.015
- Miliku, K., & Azad, M. B. (2018). Breastfeeding and the Developmental Origins of Asthma: Current Evidence, Possible Mechanisms, and Future Research Priorities. Nutrients, 10(8), 995. https://doi.org/10.3390/nu10080995
- WebMD (n.d.). Docosahexaenoic Acid (Dha) – Uses, Side Effects, and More. Retrieved July 8, 2023, from https://www.webmd.com/vitamins/ai/ingredientmono-864/docosahexaenoic-acid-dha
- American Family Physician (AAFP) (2018, August 15). Nutrition in Toddlers. Retrieved July 8, 2023, from https://www.aafp.org/pubs/afp/issues/2018/0815/p227.html
- American Diabetes Association (n.d.). Breastfeeding and Diabetes. Retrieved July 8, 2023, from https://diabetes.org/diabetes/gestational-diabetes/diabetes-breastfeeding
- U.S. Department of Agriculture-Food and Nutrition Service (2016, July 14). Nutrition Requirements for Fluid Milk and Fluid Milk Substitutions in the CACFP, Q&As. Retrieved July 8, 2023, from https://www.fns.usda.gov/cacfp/nutrition-requirements-fluid-milk-and-fluid-milk-substitutions-cacfp-qas